The eyebrows play a vital role in an individual’s appearance. The descent of the eyebrow in youth or as one ages produces a tired look and causes a fullness to the upper eyelids. Physicians have devised many procedures, such as the Beverly Hills browlift, to elevate the eyebrows in order to improve one’s appearance, and often times alleviate the need to perform upper eyelid surgery.
Cosmetic eyebrow elevating procedures, or brow lifts, have traditionally involved large incisions, usually from ear to ear, with extensive surgery and post-operative rehabilitation. While excellent results have been obtained with this technique, patients have often developed redness, irritation, itching, and loss of hair along the incision site. In addition, significant, although temporary, loss of sensation to the forehead and scalp may occur.
Endoscopic brow elevation is the most current and state-of-the art method of forehead and eyebrow lifting. The procedure, which is minimally invasive when compared to traditional surgery, involves making very small incisions behind the hairline and uses a specialized lighting system and camera to perform surgery. With this technique, post-operative rehabilitation is simpler, and the time necessary to get back to normal daily activities is greatly reduced. Most importantly, surgical results have been extremely successful and patient satisfaction has been very high from Los Angeles brow lifts.
Patient Indications
- Droopy brow and/or furrowed lines above the nose.
- Overhanging brow affecting appearance of the upper eyes.
Procedure
- Three very small, puncture-type incisions are made in the hairline. The endoscope (a mini TV camera with a probe attached) helps guide the surgeon to weaken the muscles that produce frown lines and reposition the eyebrows to a higher level.
Recovery
- To minimize swelling after a browlift, the head needs to be elevated for several days following surgery.
- Following your browlift surgery, discomfort is minimal and easily controlled by oral medication.
- Some swelling is inevitable, even around the eyes and cheeks. Bruising and swelling should begin to disappear in a week or so.
- Surgical staples are removed in seven days.
Intended Result
- A natural, younger and more rested looking appearance.
- Elevated and properly positioned eyebrows.
- Diminished frown lines.
Rejuvenation of the Aging Brow and Forehead
by Paul S. Nassif, M.D., F.A.C.S. and J. Regan Thomas, M.D., F.A.C.S.
Proportions of the Aesthetic Brow and Forehead
The forehead, from the eyebrows to the hairline, makes up the upper third of the face. The aesthetically favored forehead produces a gentle convexity on profile. Other shapes include sloping, flat and protruding. The eyebrows generally follow a smooth, gently curving arc that extends from the lateral eyebrow around the nasion and down the lateral nasal sidewall. In women, the eyebrow should lie slightly above the supraorbital rim and follow a gently curving arc. The eyebrow begins at a line drawn from the alar-facial groove through the medial canthus and ends at a line drawn from the alar-facial groove through the lateral canthus. In females, the highest point of the eyebrow arc is at a line drawn tangential to the lateral limbus. The medial and lateral ends of the eyebrow should lie in a horizontal line. The medial end should have a club like configuration that gradually tapers laterally. In men, the brow usually lies at the level of the supraorbital rim.
The Aging Brow and Forehead
Although different regions of the face age at variable rates and are influenced primarily by genetic factors, the upper third of the face ages in its own unique fashion. As skin elasticity declines, the forehead, temple and glabellar skin descends. The brow, especially in its temporal aspect, descends to or below the supraorbital rim with the effects of gravity causing temporal hooding. If brow ptosis is severe, a visual deficit may develop in the superior and temporal quadrant. The supratarsal crease disappears by over-hanging ptotic upper eyelid skin. Crow’s feet (rhytids at the lateral canthus) appear secondary to gravity and repeated contraction of the orbicularis oculi muscle. Deep forehead creases appear due to the repetitive actions of the primary brow elevator, the frontalis muscle, in an effort to elevate the heavy, ptotic brow. Vertical, oblique and horizontal rhytids appear in the glabella and nasion from contractions of the brow depressors, the corrugator, procerus and depressor supercilii muscles.
Patient Selection
Psychological Considerations
As with any facial plastic surgery procedure, careful patient selection is paramount. Realistic expectations and proper motivations of the patient are extremely important in achieving a successful outcome, a satisfied patient and a pleased facial plastic surgeon. If the surgeon despite a visually pleasing surgical result does not perform proper patient screening, patient dissatisfaction may be encountered. Educating patients about the different surgical procedures and goals requires excellent physician-patient communication and guidance. Computer imaging of the proposed brow elevation may enhance in the communication of your surgical goals since few patients are aware that brow ptosis is responsible for their orbital changes. Often, patients think and are told that droopy eyelid skin in the presence of a ptotic brow is the etiology of their “saddened” look. If upper blepharoplasty is performed in this situation, the eyebrow-lid margin is potentially narrowed, obliterating adequate delineation of the supratarsal anatomy by sacrificing excessive upper eyelid skin2. Following the education process, candidates for aging brow surgery must have informed consent with discussing possible adverse outcomes, complications and risks of the selected surgical procedure.
Anatomic Considerations
Analysis of the upper third of the face, from the eyebrows to the hairline, should begin with the assessment of interpersonal factors that may significantly affect the patient’s interpretation of successful surgical intervention and, as such, must be carefully examined. Age, gender, race, body habits and personality are the main interpersonal components that must receive consideration when assessing the eyebrow complex.
When determining what brow lifting procedure should be employed, specific anatomic criteria should be evaluated when examining the patient. The patient should be examined in a sitting position and in facial repose. Manually elevating the brow will reveal the favorable effect of brow elevation. Individuals with ptotic eyebrows often involuntarily attempt to elevate the brow with frontalis muscle contraction. To eliminate “pseudo-elevation” of the brow, have the patient close her or his eyes and then slowly open up their eyes after allowing the frontalis muscle to relax. The true position of the eyebrow can than be evaluated in repose by the surgeon. Additionally, the eyebrow position can be examined with the eyes closed. Listed below are anatomic and physiologic factors that needs to be evaluated when considering a patient for aging forehead rejuvenative surgery:
- Location of frontal and temporal hairline
- Quality of hair: alopecia, thinning or abundant hair
- Forehead height relative to facial proportions
- Severity of forehead, temporal and lateral canthal (crow’s feet) rhytids
- Eyebrow aesthetics: shape, symmetry, quality, texture, position and mobility
- Presence of prominent supraorbital ridge or hollow orbit
- Degree of dermatochalasis: excess skin, tone, lateral canthal hooding and presence of medial fat pad
- Previous eyelid or eyebrow surgery and scars
- Presence of lagophthalmos (inability to close the upper eyelid completely)
- Scalp mobility
- Lateral canthus position
- Skin elasticity and texture
- History of ocular disease or dry eyes
Surgical Goals
The goals associated with rejuvenation surgery of the brow and upper third of the face include the following.
- Elevation of ptotic eyebrows
- Reduction of lateral hooding and redundant upper eyelid skin
- Elevation of lateral canthus (if needed)
- Reduction of glabellar and corrugator rhytids
- Reduction of transverse forehead rhytids
- Reduction of lateral canthal “crow’s feet” rhytids
- Correction of eyebrow asymmetry
In general, the selected brow elevation procedure should be performed before upper blepharoplasty so that the facial plastic surgeon can judge the precise amount of upper eyelid skin to be removed. This helps prevent excessive elevation of the brow-lid complex with the potential for causing lagophthalmos. In some cases, the need for upper blepharoplasty may be eliminated after the Beverly Hills brow lift procedure has been performed.
Overall, selection of the specific brow procedure will be determined by integrating the psychological and anatomic considerations together with the proposed surgical goals.

Surgical Techniques
Traditional methods of forehead and brow rejuvenation, such as coronal, pretrichal and direct brow lifts have provided facial plastic surgeons with effective brow elevation for many years. In the past decade, the endoscopic forehead and brow lift has rapidly become accepted as part of the surgical armamentarium and is frequently the technique of
choice5,15,18. The indications and contraindications for each forehead and brow lifting procedure are described in Table 117.
Coronal Forehead Lift
For total forehead and brow elevation with excellent longevity, the coronal lift should be considered. The coronal incision is posterior to the frontal and temporal hairline, generally following the shape of the hairline, and extends from the superior helical of one ear to the other ear. The subgaleal plane is used for the dissection. Redundant and excess skin and galea is excised and the wound is closed in layers. Typically 4-0 absorbable sutures are used in the galeal layer and the skin is closed with skin staples. All aspects of the aging forehead and brow, including rhytids and ptosis, are effectively treated with this approach.
Pretrichal Forehead Lift
In patients with an elongated forehead and high hairline, the pretrichal forehead lift may
be used. The pretrichal incision created in an irregularized pattern is located at the junction of the cephalic aspect of the forehead and hairline or is placed just within the hairline to further camouflage the scar. A beveled incision is used to allow hair follicle growth through the scar adding additional camouflage. The temporal component of the incision is connected to the pretrichal incision and is posterior to the temporal hairline similar to a coronal lift. Excess skin and galea are resected from the anterior flap. Closure is beveled to accommodate the hair follicle growth through the scar. The galeal and dermal layers are closed with 4-0 absorbable suture and the skin is closed with 6-0 minimally reactive suture which is removed in one week.
The advantage of the pretrichal incision is that the forehead is not elevated and the frontal hairline is preserved. The pretrichal forehead lift treats all aspects of the aging forehead and brow.
Midforehead Lift
The midforehead lift is being performed rarely. The typical patient must have prominent forehead creases since the incision and ultimate scar is placed in an elongated, central transverse rhytid that crosses the midline. The subcutaneous plane is used for the dissection.
Midforehead Brow Lift
The midforehead brow lift is similar to the midforehead lift except that the forehead incisions are bilateral and do not cross the midline nor interconnect. Forehead and glabellar rhytids are not treated with this brow lifting procedure. The procedure may be unilateral as in cases of hemi-facial paralysis with brow ptosis on one side.
Direct Brow Lift
In certain situations, the direct brow lift may be used. The incision follows the eyebrow and is placed within and parallel to the uppermost hair follicles of the brow. Even in the best of meticulous closures, the fine scar may be visible. This procedure may also be useful in the facial paralysis patient.
Browpexy
Following the standard blepharoplasty excision of skin and orbicularis muscle, the dissection is extended superiorly toward the brow in the sub muscular postorbicularis plane1. Dissection should extend approximately 1-1.5 cm above the superior orbital rim. One to three 4-0 permanent sutures are passed transcutaneously from the lower edge of the brow hairs into the previously dissected sub-brow space approximately 1 cm apart. This transcutaneous introduction of the sutures allows the surgeon to mark the position of the brow hairs while working underneath the dissected flap.
Each suture is then passed through periosteum approximately 1-1.5 cm above the supraorbital rim. At this stage of the procedure, the height and curvature of the brow can be adjusted according to the patient’s gender. Placing the more central suture slightly higher allows the characteristic arch of the female brow to be restored or preserved.
The sutures are then passed again into the sub-brow muscular tissue at the level of the original, transcutaneously passed marking suture. It is important to engage into firm muscular-subcutaneous tissue with each suture and avoid suturing into superficial sub-brow tissue to avoid dimpling of the skin.
The original transcutaneous suture ends are then pulled through the skin under the flap. The surgeon ties the suture in a loop over a 4-0 silk knot, releasing the suture if adjustment is necessary. Care is taken to avoid over tightening the suture once adequate placement is achieved, which may immobilize the brow. The upper lid blepharoplasty incision may then be closed.
Endoscopic Brow Lift
Endoscopic brow-lifting techniques have been progressively refined through experience and improvements in equipment 5,15,18 In general, the temporal dissection and temporal fixation have been standardized; however, different options for forehead dissection are available. Subperiosteal dissection with release (elevation, incision and spread) of periosteum or subgaleal dissection and release of brow depressor musculature to the supraorbital rim are both effective techniques used in endoscopic brow lifts9. Methods of bony fixation remain a controversial topic since there are numerous methods. Some of these methods include absorbable and non-absorbable screws5, bone tunnels with sutures, fixation to soft tissue using absorbable attachment devices such as Endotine (Coapt Systems, Inc., Palo Alto, California) and fibrin glue3,7. The primary author (PSN) advocates deep temporal fixation only (DTFO) without any bone fixation10.
The technique that achieves excellent brow elevation is release of the periosteum from one inferolateral orbit to the other and release of the brow depressor musculature (corrugator, procerus, depressor supercilii and supraorbital orbicularis oculi)4,9,11. Following the brow lift in Los Angeles, all depressor vector forces should be eliminated to promote the maintenance of the newly elevated brow position since periosteal reattachment to bone takes approximately 6-12 weeks16.
Temporal Lift
Patients with adequate medial brow position and ptotic lateral brow and lateral canthal hooding, an endoscopic temporal (temple) lift may be performed. A temporal lift is performed with the same principles and technique as the endoscopic brow lift (surgical technique described below) except that the medial border of the periosteal and brow depressor musculature release is the supraorbital neurovascular complex. The supraorbital orbicularis oculi muscle is the only brow depressor treated. The medial brow and glabellar region is not dissected resulting in elevation of the lateral two-thirds of the brow-lateral canthal complex.
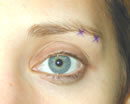 Figure 6
Figure 6
Supraorbital orbicularis oculi Botox injection sites (X). Two injections totaling 4 units. (Adapted from Zimbler MS, Nassif PS: Adjunctive applications for botulinum toxin in facial aesthetic surgery, Facial Plast Surg Clin North Am (In Press); with permission.)
Treatment of the Depressor Muscles with Botulinum Toxin
Botulinum toxin may be used synergistically with the surgical brow depressor musculature release in an effort to weaken the inferior vector forces and promote the maintenance of the newly el evated brow. Botulinum toxin is used to block the depressor function of the corrugator, procerus, depressor supercilii and lateral supraorbital orbicularis oculi muscles19. Two weeks prior to surgery, patients are injected with botulinum toxin. The corrugator, procerus and depressor supercilii muscles (medial brow depressors) are typically injected with a total of 18 units of botulinum toxin and the lateral supraorbital orbicularis oculi muscles (lateral brow depressor) are injected with about 4 units of botulinum toxin on each side (Figure 6). No botulinum toxin is injected into the frontalis muscle since it acts as the only brow elevator.
Surgical Technique
Following photo documentation of the patient’s forehead and brows, the patient is brought into the operating suite. In most situations, an anesthesiologist administers general anesthesia with a laryngeal mask
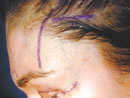 Figure 6
Figure 6
Marking of the temporal incision parallel to the tail of the brow with its medial extent at the temporal conjoint fascia.
Incisions
The incisions are then marked: 1 midline and 2 temporal (2 paramedian incisions are made if bone fixation is to be performed). The anteroposterior midline incision is approximately 2 cm posterior to the hairline and is 1 cm in length, just large enough to allow the introduction of periosteal elevators into the subperiosteal space. The temporal incisions are 3 cm in length and are approximately 2 cm posterior to the hairline. The key to obtai n a natural looking brow is to create a temporal incision parallel to the tail of the brow with its medial extent at the temporal conjoint fascia (Figure 7). The temporal incision orientation will help elevate the lateral half of the brow in a superolateral vector.
Local Anesthesia
The local anesthesia consists of 15 cc’s of 1% Lidocaine with 1:100,000 Epinephrine injected into the corrugator, procerus and depressor supercilii muscles, the proposed incision sites and for supraorbital and supratrochlear nerve blocks. The rest of the central forehead, parietal scalp, and the temporal region are infiltrated with approximately 50 cc’s of a solution consisting of 500 cc of normal saline mixed with 0.5 cc’s of 1:1000 Epinephrine, 5 cc’s of sodium bicarbonate and 25 cc’s of 2% Lidocaine without epinephrine. The high volume of the above solution acts as a vascular tourniquet with it primarily used in the temporal region. The patient is prepped and draped in the usual sterile fashion. Approximately 15 minutes is allowed for anesthesia and hemostasis to take place.
Dissection Over Frontal and Parietal Bones
The midline vertical incision is made was made and extended through the periosteum. Without the use of the endoscope, a periosteal elevator is used to create a subperiosteal pocket posteriorly over the parietal forehead and anterioly over the central forehead to approximately 1 cm above the brow with care not to injury the supraorbital and supratrochlear neurovascular bundles.
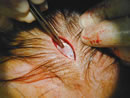 Figure 8
Figure 8
The temporal incision has been made and taken down to the deep temporal fascia.
 Figure 9
Figure 9
Endoscopic photograph of dissection over the deep temporalis fascia (large arrow) exposing the sentinel vein.
Temporal Dissection and Release of the Periosteum and Lateral Supraorbital Orbicularis Oculi Muscle
The temporal incisions are made and extended to the deep temporal fascia (Figure 8). A blunt elevator dissects over the deep temporal fascia inferiorly until a branch of the zygomaticotemporal vein called the “sentinel vein” is encountered (Figure 9). This is the inferior limit of the dissection without the use of the endoscope. A facelift scissors is used to connect the temporal incision to the central forehead incision by severing the temporal conjoint fascia (fusion of the galea and the temporoparietal fascia). The conjoint fascia is released with a periosteal elevator in an inferior direction to the level of the supraorbital rim. Near the supraorbital rim, a thickening of periosteum termed the conjoint tendon is incised sharply or bluntly. Adequate release of the conjoint tendon at the lateral supraorbital rim is an essential factor of the periosteal release.
The endoscope is placed into the temporal dissection along with the elevator visualizing the sentinel vein. This vein is a reliable marker for the frontal branch of the facial nerve, which lies superficial to the dissection on the undersurface of the temporoparietal fascia6,13. If possible, the sentinel vein is preserved and the dissection is performed medial and inferior to the vein. If the vein is cauterized, the bipolar forceps are placed at the base of the sentinel vein to help prevent a thermal neuropraxic injury to the frontal branch of the facial nerve. Lateral and slightly inferior to the sentinel vein, the zygomaticotemporal sensory nerve is encountered and is usually considered the lateral border of the dissection.
Continuing dissection in a medial diagonal direction towards the malar eminence over the superficial temporal fat pad, the periosteum is penetrated just inferomedial to the lateral canthus over the frontal process of the zygoma and malar eminence. To prevent elevation of the lateral canthus, an assistant places their finger in the interior aspect of the lateral rim at the lateral canthus(Figure 10). If the surgical plan calls for lateral canthal angle elevation, the lateral canthus is released. The periosteal release (elevation, incision and spreading) begins inferior to the lateral canthus onto the medial malar eminence and extends medially to the supraorbital neurovascular complex with care not to injure the nerve. Following the periosteal release, the lateral supraorbital orbicularis oculi muscle is meticulously released from the inferomedial orbit to the supraorbital nerve, exposing the yellow brow fat. This same procedure is performed on the contra lateral temporal region.
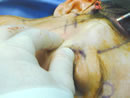 Figure 10
Figure 10
To prevent elevation of the lateral canthus, the surgeon or the assistant places a finger in the interior aspect of the lateral rim at the lateral canthus.
Release of the Brow Depressor Muscles
For the temporal lift, this portion of the procedure is eliminated. The endoscope remains placed through the temporal incision and the periosteal elevator is placed through the central incision. The dissection is carried to the central supraorbital region and radix of the nose releasing the periosteum, avoiding injury to the supraorbital and supratrochlear nerves. Thorough corrugator, procerus and depressor supercilii myotomies are performed. To ensure that complete myotomies have been performed, each nerve of the supratrochlear and supraorbital neurovascular complexes (Figure 11) should be easily visualized without obstruction from overlying muscle fibers. Finally, harvested deep temporalis fascia placed at the myotomy site of the corrugator muscles may prevent reanastomosis of muscle fibers.
 Figure 12a
Figure 12a
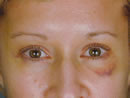 Figure 12b
Figure 12b
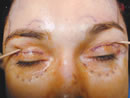 Figure 12c
Figure 12c
Intraoperative photograph of the patient’s elevated brow complex to an unnaturally high position after a complete release of all periosteum and brow depressor musculature prior fixation.
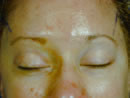 Figure 13
Figure 13
Intraoperative photograph of a patient’s elevated left brow complex after a unilateral complete release of all periosteum and brow depressor musculature prior to fixation. Q – tips positioned at the inferior border of the supraorbital rim.
Brow Elevation and Fixation
In males and in patients with a moderate amount of bleeding, a drain is placed for approximately 24 hours. If a complete release of all periosteum and brow depressor musculature is performed, the entire brow complex will elevate to an unnaturally high position without any tension (Figures 12 A-C and 13). Brow fixation is achieved by securing the superficial temporal fascia medially to the deep temporal fascia in a superolateral vector with 2 2-0 PDS horizontal mattress sutures while the brow is lifted laterally and over-corrected. The over-corrected brow will gradually drop to its final position after 3 weeks. The incisions are closed with surgical staples.
Post-operative Care Principles
Incisions are dressed with antibiotic ointment without a head dressing. Patients may experience headaches and minimal pain initially. Shampooing with gentle cleaning of the hair occurs at 48 hours, when the hair may be blow-dried on a cool setting. For 4 days, the patients are instructed to maintain a semi-upright position when sleeping or resting. The staples are removed at 7 days. Full activities may resume in 3 weeks
Complications
Few complications result from brow lifting. It has been our experience that fewer complications occur with the endoscopic brow lift as compared with the coronal lift. Hematoma, seroma, hypesthesia, tingling, pruritis, “band-like” forehead sensation, temporary frontal branch of the facial nerve paresis, temporary or permanent alopecia, infection, stitch abscess, brow asymmetry, relapse of brow ptosis, paramedian incision depressions with screw fixation, hypertrophic scars have been reported10,17.
References
- Bowman CB, Tanenbaum M, McCord CD: Internal brow lift: browplasty and browpexy. In Putterman AM, Warren LA, editors: Cosmetic oculoplastic Surgery: eyelid, forehead, and facial techniques, ed 3, Philadelphia, 1999, W.B. Saunders.
- Castanares S: Forehead wrinkles, glabellar frown and ptosis of the eyebrows, Plast Reconstr Surg 34:406, 1964.
- Cousin JN, Ellis DA: Fibrin glue as the sole fixator in endoscopic forehead lift, Presented at the Canadian society of Otolaryngology – Head & Neck surgery annual meeting, Toronto, Ontario, May 30, 2000
- De La Fuente A, Santamaria AB: Facial rejuvenation: a combined conventional and endoscopic assisted lift, Aesthetic Plast Surg 20:471-479, 1996.
- Isse NG: Endoscopic facial rejuvenation: endoforehead, the functional lift: case reports, Aesthetic Plast Surg 18:21-29, 1994.
- Larrabee WF, Makielski KH, Cupp C: Facelift anatomy, Facial Plast Surg Clin North Am 1:135-152, 1993.
- Marchac D, Ascherman J, Arnaud E: Fibrin glue fixation in forehead endoscopy: evaluation of our experience with 206 cases, Plast Recon Surg 100:704, 1997.
- Nassif PS, Kokoska MS: Aesthetic facial analysis, Facial Plast Surg Clin North Am 7(1):1, 1999.
- Nassif PS, Kokoska MS, Cooper P, et al.: Comparison of subperiosteal vs subgaleal elevation techniques used in forehead lifts, Arch Otolaryngol Head Neck Surg 124(11): 1209-1215, 1998.
- Nassif PS, Massry GG: Endoscopic brow lift: is bone fixation necessary?, Presented at the Seventeenth Annual Symposium on the Latest Advances in Cosmetic Surgery of the Face, Newport Beach, California, August 8, 2003.
- Oslin B, Core GB, Vasconez LO: The biplanar endoscopically assisted forehead lift, Clin Plast Surg 22:633-638, 1995.
- Pitanguy I: Indications and treatment of frontal and glabellar wrinkles in an analysis of 3,404 consecutive cases of rhytidectomy, Plast Reconstr Surg 67:157- 166, 1981.
- Pitanguy I, Ramos AS: The frontal branch of the facial nerve: the importance of its variations in face lifting, Plast Reconstr Surg 38; 352-356, 1966.
- Rafaty FM, Brennan HG: Current concepts of browpexy, Arch Otolaryngol 109:152, 1983.
- Ramirez OM: Endoscopic subperiosteal browlift and facelift, Clin Plast Surg 22:639-660, 1995.
- Sclafani AP, Fozo MS, Romo T, et al.: Strength and histological characteristics of periosteal fixation to bone after elevation, Arch Facial Plast Surg 5:63, 2003.
- Tardy ME, Thomas JR, Brown R: Facial aesthetic surgery, ed 1, St Louis, 1995, Mosby.
- Vasconez LO, Core GB, Gamboa-Bobadilla M, et al.: Endoscopic techniques in coronal brow lifting, Plast Reconstr Surg 94:788-793, 1994.
- Zimbler MS, Nassif PS: Adjunctive applications for botulinum toxin in facial aesthetic surgery, Facial Plast Surg Clin North Am (In Press).
(This article was published in OTOLARYNGOLOGY: HEAD AND NECK SURGERY, 4/E Nassif PS, Thomas PS, Rejuvenation of the Aging Brow and Forehead, 750-763, Copyright 2005 Mosby, and is posted with permission from Elsevier. Copies of the article can be downloaded and printed only for the reader’s personal research and study.)
Visit Cummings: Otolaryngology online at http://www.us.elsevierhealth.com/product.jsp?isbn=0323019854
Table
Adapted from Forehead-lift. In Tardy ME, Thomas JR, Brown R, editors: Facial aesthetic surgery, ed 1, St Louis, 1995, Mosby p 163.
(Procedure in left column, Indications and Advantages in middle column, and Contraindications and Disadvantages in right column)
| Procedure | Indications and Advantages | Contraindications and Disadvantages |
|
|
||
| Coronal forehead lift | • Treats all aspects of the aging forehead and brow | • Limited use in males • Elevates hairline • Vertically lengthens upper third of face • Elongated scar • Possible prolonged hypesthesia of scalp • Less fine-tuning of brow position |
|
|
||
| Pretrichal forehead lift | • High hairline • No vertical forehead lengthening • Preserves the hairline • Treats all aspects of the aging forehead and brow |
• Possible visible (exposed) scar • Possible prolonged hypesthesia of scalp |
|
|
||
| Midforehead lift | • Prominent horizontal forehead creases • Preserves the hairline • Improved fine-tuning of brow position • Corrects brow asymmetry |
• Possible visible (exposed) scar • Avoid in oily, thick skin |
|
|
||
| Midforehead brow lift | • Prominent horizontal forehead creases • Improved fine-tuning of brow position • Corrects brow asymmetry |
• Possible visible (exposed) scar • Treats brows only • Avoid in oily, thick skin |
|
|
||
| Direct brow lift | • Accurate brow elevation • Preserves forehead/scalp sensation • Patients with abundant or thick brow hair preferred • Immediate scar camouflage (with hair) • Corrects brow asymmetry |
• Possible visible (exposed) scar • Treats brows only |
|
|
||
| Temporal lift | • Ideal and immediate scar camouflage (with hair) • Improves lateral hooding |
• Not useful for midforehead glabellar creases • No effect on medial aspect of brow |
|
|
||
| Browpexy | • Performed through the upper blepharoplasty incision • Indicated for mild brow ptosis |
• Possible prolonged eyelid edema • Possible brow asymmetry • Possible unsatisfactory results |
|
|
||
| Endoscopic brow lift | • Less invasive with small incisions • Excellent scar camouflage • High hairline • No vertical forehead lengthening • Preserves the hairline • Treats most aspects of the aging forehead and brow |
• Less fine-tuning of brow position • Possible depressions in the soft tissue of the scalp due to screw fixation |
Paul S. Nassif, M.D., F.A.C.S. is a world-renowned facial plastic and reconstructive surgeon whose work has been featured on numerous international and national television and print media. He has been featured on such programs as NBC World Nightly News with Tom Brokaw, ABC World News Tonight with Peter Jennings, CBS’ The Early Show, CNN, MSNBC, E!, EXTRA!, VH1, BBC, The Learning Channel and Discovery Health. Dr. Nassif has also been quoted in such publications as the New York Times, Associated Press (world-wide), The Wall Street Journal, USA Today, and Los Angeles Times among others.
For a complete list of his media work, go to the Media section.
© Spalding Drive Plastic Surgery. All rights reserved. Web Design & Online Marketing Los Angeles by Studio III